Gum Diseases and Systemic Health

Gum Diseases and Systemic Health
For many years the mouth was viewed as separate to the rest of the body, but of course it isn’t. Research investigating the systemic effects of periodontitis has shown that there is a two-way relationship between Diabetes Mellitus (Figure 6A), Cardiovascular Diseases (Figure 6B), Rheumatoid Arthritis (Figure 6C) as well as adverse Pregnancy outcomes (Figure 6D). In addition, Obesity may affect Periodontal Disease (Figure 6E). This page provides an overview of these interaction.
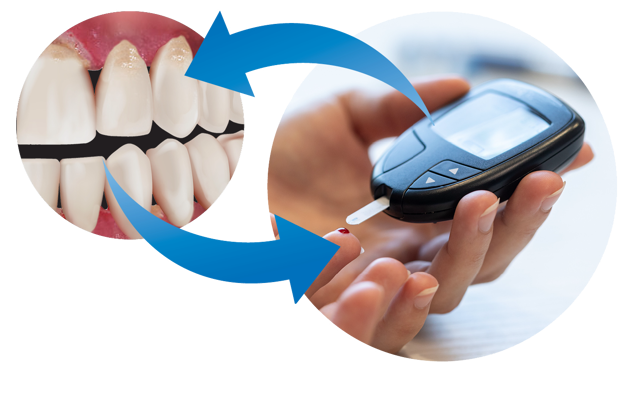
Diabetes Mellitus (DM)
Diabetes Mellitus (DM) is a chronic condition caused by relative or absolute insulin deficiency, which results in hyperglycaemia. Long-term complications of diabetes include kidney disease, retinopathy, neuropathy, and cardiovascular disease. Diabetes is a known risk factor for periodontal disease and poor glycaemic management is related to the severity of periodontal disease. Patients with diabetes who have periodontitis may have poorer glycaemic control and an increased risk of diabetic complications. A two-way relationship between periodontal disease and DM has been shown. However, exactly how diabetes affects periodontal disease and vice versa remains incompletely understood. Both diseases are associated with chronic inflammation. It is currently suggested that an increase in inflammation from one may exacerbate the other. Interestingly, patients with periodontitis can be pre-diabetic or undiagnosed diabetics. As a result, a dentist or periodontist may send a patient for a glucose test. Lastly, the treatment of periodontitis in patients with diabetes has been shown to make a small improvement in glycaemic control. Patients with diabetes need to be aware of the increased likelihood of periodontal disease.
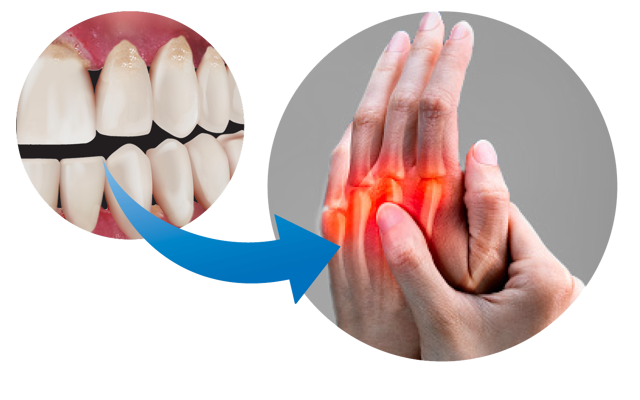
Rheumatoid Arthritis (RA)
Rheumatoid Arthritis (RA) is an autoimmune disease primarily affecting the lining of the joints, which become inflamed and sore. Fatigue is also quite commonly reported. Patients with RA are more likely to have severe periodontal problems and vice versa. A flare-up of RA may exacerbate periodontitis and well controlled RA may improve periodontal health. The two diseases have very similar inflammatory processes and this or the increase in inflammation may be the reason for the two-way relationship. Recently it has been proposed that conversion of arginine to citrulline by the bacteria involved in periodontitis may result in an immune reaction leading to autoimmune diseases such as RA.
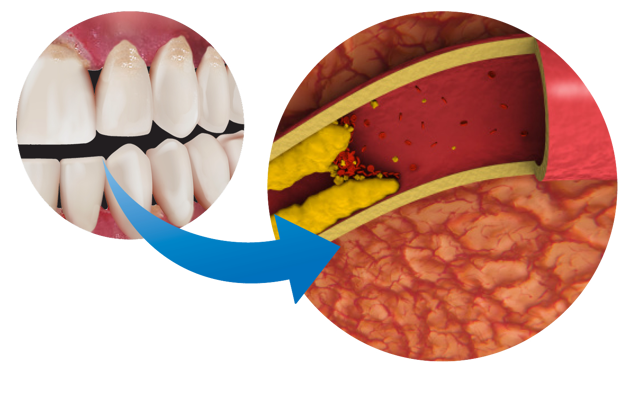
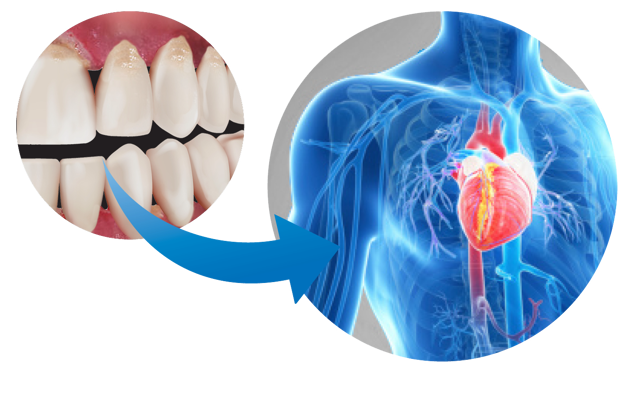
Cardiovascular Diseases (CVD)
Cardiovascular Diseases (CVD), such as coronary heart disease or high blood pressure (hypertension), have also been linked to periodontal diseases. CVD is a major cause of death in Australia with a substantial percentage of the population having at least one cardiovascular condition. The prevalence of CVD is higher in patients with periodontal disease and vice versa. Many of the risk factors for both diseases are similar and include age, gender, ethnicity, socio-economic status, smoking and stress. There may also be genetic susceptibility which predisposes to both CVD and periodontitis. Every time people with periodontitis brush their teeth, they most likely release the bacteria that cause gum disease into the blood stream. This and the increased inflammation from periodontitis may cause damage to the systemic circulation by impairing blood vessel function, promoting formation of atheroma or fatty plaques in the arteries and increasing the risk of thrombotic and embolic events, such as a myocardial infarction. However, the effect of treatment of periodontal disease on CVD is either very low or not shown. That said it is important that periodontal health is maintained in people with CVD.
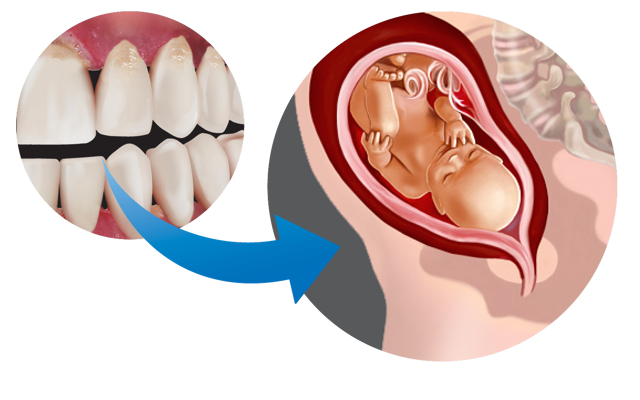
Adverse Pregnancy Outcomes
Adverse pregnancy outcomes include pre-term birth, which occurs when a baby is born before 37 weeks of pregnancy, and low-birth weight, a birth weight less than 2.5kg. Infection, smoking, problems during pregnancy and nutrition influence low birth weight. Low birth weight is associated with chronic diseases later in life. Periodontitis has been linked with pre-term and low birth weight due to the increased inflammation and the bacteria causing periodontal disease to have been found in amniotic fluid. Periodontitis can also reduce fertility. Treating periodontal disease during pregnancy does not appear to reduce the likelihood of pre-term or low birth weight, but the research has shown that treatment during semester 2 is safe. Ideally if one is planning on getting pregnant periodontal disease should be managed beforehand.
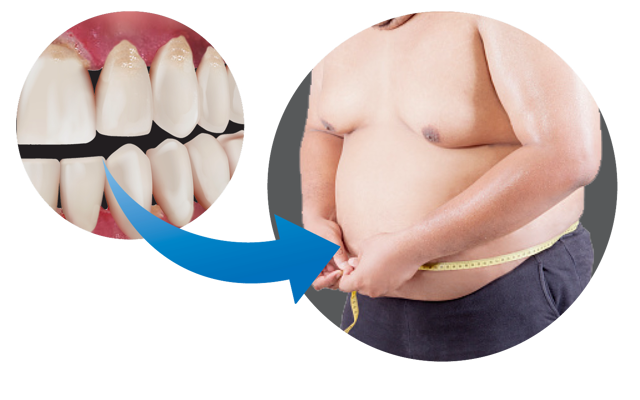
Obesity
Obesity is the accumulation of excess body fat. A Body Mass Index of over 25 is considered overweight and above 30 obese. Obesity increases your risk of other diseases and health problems, such as heart disease, diabetes and high blood pressure. Obese patients are more likely to have periodontal disease and obesity has recently been recognised as a factor increasing the risk for periodontitis. The link between periodontitis and obesity may be linked to lifestyle, such as smoking, poor oral hygiene, or lack of dental visits. It is known that obesity is also a chronic inflammatory state and again inflammation from one or the other may predispose or exacerbate the other.